Cytomegalovirus
Check with your physician regarding your CMV status prior to placing an order. (See discussion below.)
CMV is a virus that most American adults have been exposed to and have immunity to. In healthy adults and children it produces mild cold or flu like symptoms for 1-2 weeks. If a woman who has never had CMV becomes infected with the virus during pregnancy, the child is at risk for developing severe medical problems, such as mental retardation, deafness and seizures. You can be tested to determine if you have been exposed to CMV. If you are CMV negative, you should consider restricting your selections to CMV negative donors, to prevent the small chance of developing CMV during pregnancy and passing it the developing child. Information on the CMV status of all donors is available on their summary profile.
DETAILED QUESTIONS AND ANSWERS REGARDING CMV
WHAT IS CMV?
Cytomegalovirus, commonly called CMV, is a member of the herpes virus family that includes chicken pox, cold sores, and infectious mononucleosis (mono). The virus is carried by people and is not associated with food, water or animals. Most individuals are exposed to CMV in childhood and have a mild infection similar to a typical cold, while the immune system develops antibodies to fight the infection. The virus remains alive, but becomes dormant, or hides, inside certain cells for the rest of the person's lifetime. Approximately 50-85% of American adults will test CMV positive, confirming exposure. In developing countries, or areas of poor sanitation, this number is almost 100%. However, in a small number of individuals, the virus may reactivate and be transmitted in bodily fluids, such as semen. This is very common in people with immune suppression or individuals that have only recently been exposed to CMV.
WHAT IS THE DIFFERENCE BETWEEN CMV IgG AND IgM TESTS?
The CMV IgG test indicates previous exposure to CMV. The CMV IgM test indicates a recent or current infection, in which case all vials are discarded.
HOW IS CMV SPREAD?
CMV is spread person-to-person by direct exposure to urine, saliva, mucus, cervical secretions, semen, blood, or breast milk. There is no vaccine for CMV. Daycare centers are one of the more common exposure settings, where children can transmit the virus through contact with each other's bodily fluids (infected children carry the virus in their respiratory and urinary tracts for long periods of time). Adults can also be infected through unprotected sexual contact. The production of virus may take place intermittently, without any detectable signs, and without causing symptoms. An infected mother can transmit CMV to her fetus either through the placenta or through exposure to her infected cervical secretions during birth.
WHAT ARE THE SYMPTOMS OF CMV INFECTION?
The symptoms are usually mild, non-specific, hard to detect, and resolve in 1-2 weeks. An adult may not even realize that they have an infection. Some people develop a 'flu-like' illness with swollen lymph nodes or they may complain of feeling tired. Children may have a runny nose. In people with impaired immune systems may develop a serious illness. Pregnant women who are infected for the first time during pregnancy usually recover completely with few or no symptoms. The unborn baby is at risk for congenital infection.
WHAT ARE THE SYMPTOMS OF A CONGENITAL INFECTION?
If a pregnant woman has never been exposed to CMV and has her first infection during pregnancy, there is a chance that the fetus could become infected before the mother's body can eliminate the virus. Transmission to the fetus only occurs in a third of women who have a primary infection during pregnancy. Congenital CMV is the most common congenital infection in the US. Twenty percent of babies born with an infection develop medical complications over the first few years of life. Those symptoms can include low birth weight, deafness, blindness, mental retardation, small head, seizures, jaundice, brittle teeth and damage to the liver and spleen. While a child may develop some of the above symptoms, no baby develops all the symptoms and some infants have no symptoms at all.
HOW DOES CRYOGENIC LABORATORIES SCREEN ITS DONORS?
Laboratory testing for antibody to CMV is performed on all donors. If the antibody test is negative or not detectable, the donor is presumed not to have been previously infected. A new test is done every three months to monitor for new infections. If the donor tests positive for antibodies, additional testing is performed to determine if the positive antibody test represents a recent or old infection. If a recent infection cannot be ruled out, all suspect semen vials are discarded.
IS IT SAFE TO USE A DONOR WHO IS POSITIVE FOR CMV?
You may wish to consult with your own medical practitioner as to whether he or she feels it is acceptable to use a donor who is positive for CMV IgG antibodies. Given our screening process, we presume that our donors who are positive for CMV IgG antibodies are non-infectious for CMV. Furthermore, our six-month quarantine policy ensures that should a donor test positive for a current or recent infection, we would destroy all his potentially infectious samples before they were ever released to recipients.
WHAT DONORS MAY I USE IF I AM CMV NEGATIVE?
We would highly recommend that you use a CMV negative donor. However, you may use a CMV positive donor, if you wish. While the risk is not zero, the chance of transmitting congenital CMV to a developing fetus from semen used at the time of conception is extremely low. This is, however, a medical issue that you should discuss with your physician.
For more information you can view the CDC website fact sheet at http://www.cdc.gov/cmv/facts.htm.
CLI Medical Report - Therapeutic Donor Insemination and Cystic Fibrosis
Background
Cystic fibrosis (CF) is the most common severe inherited disease in Caucasians. It is less frequent in individuals of African American or Asian ancestry. The disease usually begins in infancy or childhood with recurrent lung problems (including pneumonia), intestinal difficulties, or poor growth. Medications, frequent visits to physicians, and hospitalizations are almost always required. While there has been much improvement in the care of children with CF, many of them still die in early childhood, and about half of all victims of CF die in young adulthood.
 Risks
Risks
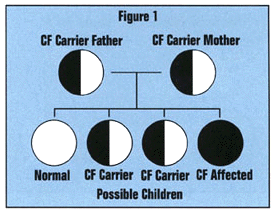
Almost any couple is at risk of having CF. Genes are passed to your child in the egg and sperm. Ordinarily you have two normal copies of a gene. If one copy of the CF gene is abnormal, you are still healthy, but are a carrier of CF. If you and your spouse are both carriers, two abnormal copies of the CF gene, one from you and one from your spouse, can be passed on to your child (See Figure 1). If you and your spouse are both carriers, you have a 1 in 4 chance that your baby will inherit two CF genes and be affected with CF. If this happens your child will have cystic fibrosis. Like most individuals, you may not realize that you may be at risk for having a child with the disease. Most CF carriers have no family history of affected children. Approximately 1 in 25 Caucasian Americans are carriers of the CF gene. One in every 2,500 Caucasian births results in a child who is affected with cystic fibrosis. Individuals whose ancestors are African or Asian can also be affected with CF, but this occurs less often. For example, in the African American population, only one out of every 17,000 births result in a child who is affected with CF.
 Testing
Testing
In1989 the gene which causes CF was discovered. This permitted development of the test that currently detects over 90% of all CF carriers. Thus, a positive test proves that you are a carrier, while a negative test greatly reduces, but does not eliminate, the risk of being a carrier.
CLI screens all prospective donors for cystic fibrosis (1) by obtaining a detailed family medical history and (2) by performing genetic testing on a sample of donor blood. The specialized testing is performed by a fully licensed/accredited genetics laboratory. All CLI donors have a negative cystic fibrosis carrier test result.
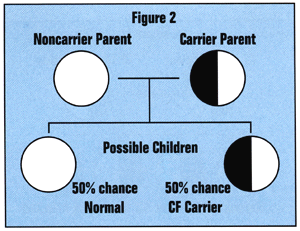
At the present time, over 1000 different changes (known as mutations) in the CF gene have been identified. Only one mutation is necessary to change a normal gene into a CF gene. The laboratory assays that are currently being used are designed to test for the most common mutations. Testing for all of the known mutations is not practical since the majority of them are very rare. At the present time cystic fibrosis carrier screening cannot provide 100% certainty that an individual is not a carrier of a CF mutation. DNA studies do not constitute a definitive diagnostic test or precise carrier test for CF in all families. Thus the interpretation of all data is usually given as a probability. If a recipient wishes further assurance of safety, CLI recommends that the recipient of donor semen be tested to determine if she is a CF carrier (See Figure 2). If an individual receives a negative result for CF carrier testing, the chance of that person being a carrier of the CF gene is significantly reduced, although not completely eliminated (See Table 1 below).
Table 1 - Likelihood Of Being A CF Carrier
| Ethnic Background |
Before Testing
(no known family history) |
After a NEGATIVE test result |
| Caucasian - Non-Jewish |
1/25 (4%) |
approx. 1/208 (0.5%) |
| Caucasian - Jewish |
1/25 (4%) |
approx. 1/833 (0.1%) |
| African American |
1/65 (1.4%) |
approx. 1/117 (0.8%) |


